Many clinics in Bali are claiming to do NAD+ infusions. However, after further research, it has been discovered that they are supplying patients with either NAD or NMN. There is a BIG difference.
The purpose of this is to educate you as a patient on the difference. While there are benefits to NMN and NAD, the + sign at the end of NDA+ is the difference between the benefits in research and outcomes.
What’s NMN?
NMN stands for nicotinamide mononucleotide, a molecule naturally occurring in all life forms. At the molecular level, it is a ribonucleotide, which is a basic structural unit of nucleic acid RNA. Structurally, the molecule is composed of a nicotinamide group, a ribose, and a phosphate group (Figure 1). NMN is the direct precursor of the essential molecule nicotinamide adenine dinucleotide (NAD+) and is considered a key component to increase NAD+ levels in cells.
What is Nicotinamide Adenine Dinucleotide (NAD+)?
NAD+ is an essential coenzyme required for life and cellular functions. Enzymes are catalysts that make biochemical reactions possible. Coenzymes are ‘helper’ molecules that enzymes need in order to function.
What Does NAD+ Do?
NAD+ is the most abundant molecule in the body besides water, and without it, an organism would die. NAD+ is used by many proteins throughout the body, such as the sirtuins, which repair damaged DNA. It is also important for mitochondria, which are the powerhouses of the cell and generate the chemical energy that our bodies use.
NAD+ Functions as a Coenzyme in Mitochondria
NAD+ plays an especially active role in metabolic processes, such as glycolysis, the TCA Cycle (AKA Krebs Cycle or Citric Acid cycle), and the electron transport chain, which occurs in our mitochondria and is how we obtain cellular energy.
In its role as a ligand, NAD+ binds to enzymes and transfers electrons between molecules. Electrons are the atomic basis for cellular energy and by transferring them from one molecule to the next, NAD+ acts through a cellular mechanism similar to recharging a battery. A battery is depleted when electrons are expended to provide energy. Those electrons can’t return to their starting point without a boost. In cells, NAD+ serves as that booster. In this way, NAD+ can decrease or increase enzyme activity, gene expression, and cell signaling.
NAD+ Helps Control DNA Damage
As organisms grow older, they accrue DNA damage due to environmental factors such as radiation, pollution, and imprecise DNA replication. According to the current aging theory, the accumulation of DNA damage is the main cause of aging. Almost all cells contain the ‘molecular machinery’ to repair this damage. This machinery consumes NAD+ and energy molecules. Therefore, excessive DNA damage can drain valuable cellular resources.
One important DNA repair protein, PARP (Poly (ADP-ribose) polymerase), depends on NAD+ to function. Older individuals experience decreased levels of NAD+. The accumulation of DNA damage as a result of the normal aging process leads to increased PARP, which causes decreased NAD+ concentration. This depletion is exacerbated by any further DNA damage in the mitochondria.
PARP1 is ‘Middleman’ of DNA Repair
Schematic of How PARP1 Helps Repair Damaged DNA
How Does NAD+ Affect Sirtuins (the Longevity Genes) Activity?
The newly discovered sirtuins, also known as the “guardian of genes,” play a vital role in maintaining cellular health. Sirtuins are a family of enzymes, participating in cellular stress responses and damage repair. They’re also involved in insulin secretion, and the aging processes and aging-related health conditions, such as neurodegenerative diseases and diabetes. The activation of sirtuins requires NAD+.
As David Sinclair, a Harvard geneticist and NAD researcher says we lose NAD+ as we age “and the resulting decline in sirtuin activity, is thought to be a primary reason our bodies develop diseases when we are old but not when we are young.” He believes that increasing NAD+ levels naturally while aging may slow or reverse certain aging processes.
Why Should We Care About NAD+
Since the discovery of NAD+ in 1906, the molecule has been on scientists’ radar for its abundance in the body and its crucial role in molecular pathways that keep our body running. In animal studies, raising NAD+ levels in the body has shown promising results in research fields like metabolics and age-related disease and has even shown some anti-aging properties. Age-related illnesses such as diabetes, cardiovascular diseases, neurodegeneration and general decreases in the immune system.
Can NMN Help Fight COVID-19
As COVID-19 swept the cities with pneumonia-like illness, infecting millions of people worldwide, scientists are on the hunt for a safe and effective cure. Gerontologist, scientists who study the biology of aging, believe that therapeutics that target aging may provide a new angle to tackle the pandemic.
Statistics have shown that COVID-19 disproportionately infects older adults. About 13.4 percent of patients 80 or older die from COVID-19, compared to 1.25 percent and 0.06 percent of those in their 50s and 20s. A recent study from the University of Oxford that analyzed 17.4 million UK adults showed age is the most substantial risk factor associated with COVID-19 death. Other risk factors include being male, uncontrolled diabetes and severe asthma.
Given the gerolavic nature – harmful to the old – of the virus, some gerontologists claim that treating “aging” can be a long term solution to defend older adults from COVID-19 and other future infectious diseases. Although more study needs to be done, a recent study listed NAD+ boosting agents such as NMN and NR as one of the potential treatments. Other scientists also hypothesized that older adults might benefit from NAD+’s longevity effects and prevent the deadly over-activation of immune responses called a cytokine storm, in which the body attacks its cells rather than the virus.
The cell uses up NAD+ during the fight against coronavirus, weakening our body, according to a recent study that has not been peer-reviewed. NAD+ is essential for innate immune defense against viruses. The researchers of the study are trying to assess whether NAD+ boosters can help humans beat the pandemic.
While scientists are in the lab racing time to find a cure for COVID-19, physicians on the front lines running out of options turn to innovative techniques. As a last resort to treat his patients, doctor Robert Huizenga of Cedars Sinai Medical Center administered an NMN cocktail infused with boosters like zinc to the patient to calm the cytokine storm stirred up by COVID-19. The NMN cocktail brought down the patients’ fever and inflammation levels within 12 hours.
During the pandemic, NMN is receiving more and more attention for its role in maintaining the immune system balance, which may be a possible treatment for the coronavirus-caused cytokine storm. With the preliminary studies showing some positive results, although not a guaranteed cure, many scientists and physicians believe the NAD+ booster’s effect on COVID-19 is worth investigating.
Aging
NAD+ is the fuel that helps sirtuins sustain genome integrity and promote DNA repair. Like a car cannot drive without fuel, sirtuins’ activation requires NAD+. Results from animal studies showed that raising NAD+ level in the body activates sirtuins and increases the lifespans of yeast, worms and mice. Although animal studies showed promising results in anti-aging properties, scientists are still studying how these results can translate to humans.
Metabolic Disorders
NAD+ is one of the keys to maintaining healthy mitochondrial functions and steady energy output. Aging and high-fat diet reduces the level of NAD+ in the body. Studies have shown that taking NAD+ boosters can alleviate diet-associated and age-associated weight gain in mice and improve their exercise capacity, even in aged mice. Other studies even reversed the diabetes effect in female mice, showing new strategies to fight metabolic disorders, such as obesity.
Heart Function
Boosting NAD+ levels protects the heart and improves cardiac functions. High blood pressure can cause an enlarged heart and blocked arteries that lead to strokes. In mice, NAD+ boosters have replenished NAD+ levels in the heart and prevented injuries to the heart caused by a lack of blood flow. Other studies have shown that NAD+ boosters can protect mice from abnormal heart enlargement.
Neurodegeneration
In mice with Alzheimer’s, raising the NAD+ level can decrease protein build up that disrupts cell communication in the brain to increase cognitive function. Boosting NAD+ levels also protects brain cells from dying when there’s insufficient blood flow to the brain. Many studies in animal models present new prospects of helping the brain age healthily, defending against neurodegeneration and improving memory.
Immune System
As adults get older the immune system declines, people get ill more easily, and it becomes harder for people to bounce back from illnesses such as the seasonal flu, or even COVID-19. Recent studies have suggested that NAD+ levels play an important role in regulating inflammation and cell survival during the immune response and aging. The study underscored the therapeutic potential of NAD+ for immune dysfunction.
How Does the Body Make Nicotinamide Adenine Dinucleotide (NAD+)?
Our bodies naturally produce NAD+ from smaller components, or precursors. Think of them as the raw materials for NAD+. There are five main precursors that occur in the body: tryptophan, nicotinamide (Nam), nicotinic acid (NA, or niacin), nicotinamide riboside (NR), and nicotinamide mononucleotide (NMN). Of these, NMN represents one of the final steps of NAD+ synthesis.
These precursors can all come from diet. Nam, NA and NR are all forms of vitamin B3, an important nutrient. Once in the body, our cells can synthesize NAD+ by several different pathways. A biochemical pathway is equivalent to a factory production line. In the case of NAD+, multiple production lines all lead to the same product.
The first of these pathways is called the de novo pathway. De novo is a Latin expression that equates to “from scratch.” The de novo pathway begins with the earliest of the NAD+ precursors, tryptophan, and builds upwards from there.
The second pathway is called the salvage pathway. The salvage pathway is akin to recycling, in that it creates NAD+ from the products of NAD+ degradation. All proteins within the body need to be regularly degraded to stop them from accumulating to unhealthy degrees. As part of this cycle of production and degradation, enzymes take some of the results of a protein’s degradation and put it right back into that same protein’s production line.
NAD+ Biosynthesis from NMN
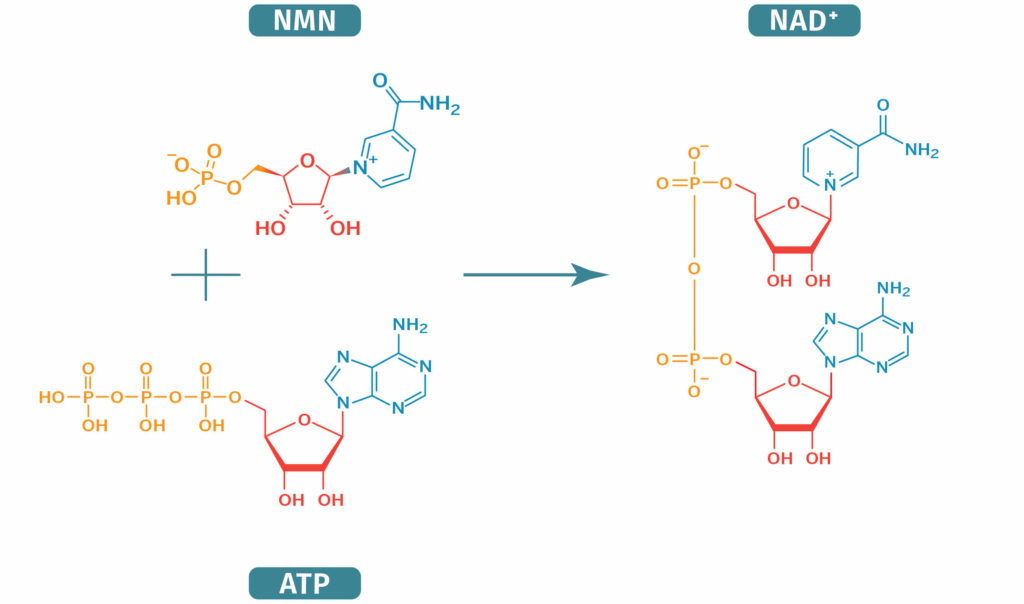
How is NMN Synthesized In the Body?
NMN is produced from B vitamins in the body. The enzyme responsible for making NMN in the body is called nicotinamide phosphoribosyltransferase (NAMPT). NAMPT attaches nicotinamide (a vitamin B3) to a sugar phosphate called PRPP (5’-phosphoribosyl-1-pyrophosphate). NMN can also be made from ‘nicotinamide riboside’ (NR) through the addition of a phosphate group.
‘NAMPT’ is the rate-limiting enzyme in the production of NAD+. This means lower levels of NAMPT cause decreased NMN production, resulting in decreased NAD+ levels. Adding precursor molecules like NMN can also speed up NAD+ production.
Methods to Increase NAD+ levels
Fasting or reducing calorie intake, better known as calorie restriction, has been shown to increase NAD+ levels and sirtuin activity. In mice, the increased NAD+ and sirtuin activity from calorie restriction has been shown to slow the aging process. Although NAD+ is present in some foods, the concentrations are too low to affect intracellular concentrations. Taking certain supplements, such as NMN, has been shown to increase NAD+ levels.
NAD Supplement as NMN
Intracellular concentrations of NAD+ decrease from aging as normal cellular functions deplete NAD+ supplies over time. Healthy levels of NAD+ are thought to be restored by supplementation with NAD+ precursors. According to research, precursors such as NMN and nicotinamide riboside (NR) are viewed as supplements of NAD+ production, increasing concentrations of NAD+. David Sinclair, an NAD+ researcher from Harvard, says, “Feeding or administering NAD+ directly to organisms is not a practical option. The NAD+ molecule cannot readily cross cell membranes to enter cells, and therefore would be unavailable to positively affect metabolism. Instead, precursor molecules to NAD+ must be used to increase bioavailable levels of NAD+.” This means NAD+ cannot be used as a direct supplement because it is not easily absorbed. NAD+ precursors are more easily absorbed than NAD+ and are more effective supplements.
How are NMN Supplements Absorbed and Distributed Throughout the Body?
NMN appears to be absorbed into cells through a molecular transporter embedded in the cell surface. Being smaller than NAD+, the NMN molecule may be absorbed more efficiently into cells. NAD+ cannot easily enter the body because of the barrier presented by the cell membrane. The membrane has a waterless space which prevents ions, polar molecules, and large molecules from entering without the use of transporters. It was once thought that NMN must be altered before entering cells but new evidence suggests that it can enter cells directly via an NMN-specific transporter in the cellular membrane.
Furthermore, injections of NMN result in increased NAD+ in many regions in the body including the pancreas, fat tissue, the heart, skeletal muscle, kidneys, testes, eyes, and blood vessels. Oral administration of NMN in mice increases NAD+ in the liver within 15 minutes.
NMN is Quickly Converted to NAD+
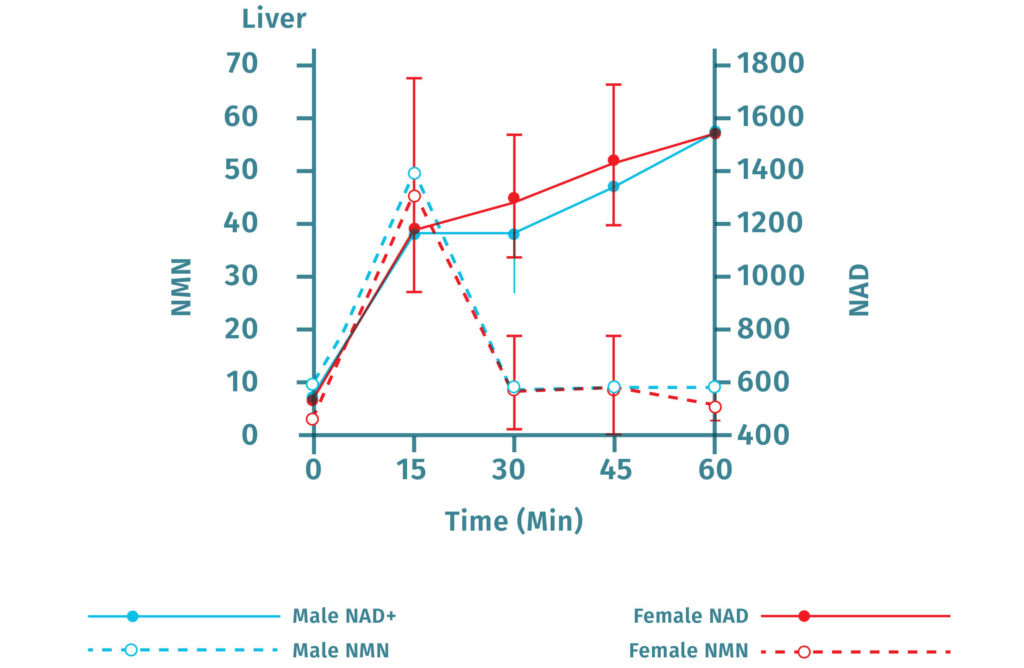
NMN Side Effects and Safety
NMN is considered safe in animals, and the results are promising enough that human clinical trials have started. This molecule is largely considered to be safe and not toxic, even at high concentrations in mice and in a human study. Long-term (one-year) oral administration in mice does not have toxic effects. The very first clinical trial in humans was completed and the evidence supports the idea that it is not toxic in single doses.
Although one study of Japanese men published in November 2019 noted that subjects had increased levels of bilirubin in their blood following NMN administration, these levels remained within the normal range. Future studies should focus on long-term safety and efficacy of usage. NMN is not associated with any other known side effects.
The History of NMN and NAD+
Nicotinamide adenine dinucleotide, or NAD for short, is one of the most important and versatile molecules in the body. Because it is central to providing cells with energy, there is almost no biological process that does not require NAD. As a result of this, NAD is the focus of widespread biological research.
In 1906, Arthur Harden and William John Young discovered a “factor” in liquid extracted from brewer’s yeast enhanced the fermentation of sugar into alcohol. That “factor,” called a “coferment” at the time, turned out to be NAD.
Harden, along with Hans von Euler-Chelpin, continued to peel apart the mysteries of fermentation. They were awarded the Nobel Prize in 1929 for developing a detailed understanding of these processes, including the chemical shape and properties of what would soon be known as NAD.
The story of NAD expanded in the 1930’s, under the guidance of Otto Warburg, another Nobel laureate, who discovered NAD’s central role in facilitating many biochemical reactions. Warburg discovered that NAD serves as a sort of biological relay for electrons.
The transfer of electrons from one molecule to another, serves as the basis for the energy needed to perform all biochemical reactions.
In 1937, Conrad Elvehjem and colleagues at the University of Wisconsin, Madison, discovered that NAD+ supplementation cured dogs of pellagra, or “Black Tongue.” In humans, pellagra causes a host of symptoms, including diarrhea, dementia, and sores in the mouth. It stems from a niacin deficiency and is now regularly treated with nicotinamide, one of the precursors to NMN.
Arthur Kornberg’s research on NAD+ throughout the 40’s and 50’ was instrumental in leading him to discover the principles behind DNA replication and RNA transcription, two processes vital for life.
In 1958, Jack Preiss and Philip Handler uncovered the three biochemical steps, by which nicotinic acid is converted to NAD. This series of steps, called a pathway, is known today as the Preiss-Handler Pathway.
In 1963, Chambon, Weill, and Mandel reported that nicotinamide mononucleotide (NMN) provided the energy needed to activate an important nuclear enzyme. This discovery paved the way for a series of remarkable discoveries on a type of protein called a PARP. PARPs play crucial roles in repairing DNA damage, regulating cell death, and whose activity is associated with changes in lifespan.
In 1976, Rechsteiner and his colleagues found convincing evidence NAD+ seemed likely to have “some other major function” in mammalian cells, beyond its classical biochemical role as an energy transfer molecule.
This discovery made it possible for Leonard Guarente and his colleagues to discover that proteins called sirtuins use NAD to extend lifespan by differentially keeping some genes “silent.”
Since then, interest has grown in NAD and its intermediates, NMN and NR, for their potential to ameliorate a number of age-related health issues.
The Future of Nicotinamide Mononucleotide
With the promising therapeutic properties that NMN showed in animal studies, researchers are aiming to understand how this molecule works in the human body. A recent clinical trial in Japan demonstrated that the molecule is safe and well-tolerated at the used dosage. More studies and human trials are on the way. It is a fascinating and versatile molecule, from which we still have much to learn. Journal Reference
- Vincenzo Carafa, Dante Rotili, Mariantonietta Forgione, Francesca Cuomo, Enrica Serretiello, Gebremedhin Solomon Hailu, Elina Jarho, Maija Lahtela-Kakkonen, Antonello Mai, Lucia Altucci. Sirtuin functions and modulation: from chemistry to the clinic. Clin epigenetics, 2016; DOI: 10.1186/s13148-016-0224-3.
- Niels J. Connell, Riekelt H. Houtkooper, Patrick Schrauwen. NAD+ metabolism as a target for metabolic health: have we found the silver bullet? Diabetologia, 2019; DOI: 10.1007/s00125-019-4831-3.
- Julia Evangelou. “Natural compound reduces signs of aging in healthy mice.” ScienceDaily.com. 27 October, 2016. Web. 16 January. 2020.
- Henryk Jęśko, Przemysław Wencel, Robert P. Strosznajder, Joanna B. Strosznajder. Sirtuins and Their Roles in Brain Aging and Neurodegenerative Disorders. Neurochem Res, 2017; DOI: 10.1007/s11064-016-2110-y.
- Ann Katrin-Hopp, Patrick Grüter, Michael O. Hottiger. Regulation of Glucose Metabolism by NAD+ and ADP-Ribosylation. Cells, 2019; DOI: 10.3390/cells8080890.
- Vamshi K.C. Nimmagadda, Tapas K. Makar, Krish Chandrasekaran, Avinash Rao Sagi, Jayanta Ray, James W. Russell, Christopher T Bever Jr. SIRT1 and NAD+ precursors: Therapeutic targets in multiple sclerosis a review. J Neuroimmunol, 2017; DOI: 10.1016/j.jneuroim.2016.07.007.
- Katalin Sas, Elza Szabó, László Vécsei. Mitochondria, Oxidative Stress and the Kynurenine System, with a Focus on Ageing and Neuroprotection. Molecules, 2018; DOI: 10.3390/molecules23010191.
- Yue Yang, Anthony A. Sauve. NAD+ metabolism: Bioenergetics, signaling and manipulation for therapy. Biochim Biophys Acta, 2016; DOI: 10.1016/j.bbapap.2016.06.014.
- Jun Yoshino, Kathryn F. Mills, Myeong Jin Yoon, Shin-ichiro Imai. Nicotinamide Mononucleotide, a Key NAD+ Intermediate, Treats the Pathophysiology of Diet- and Age-Induced Diabetes in Mice. Cell Metab, 2011; DOI: 10.1016/j.cmet.2011.08.014.
- Mills KF, Yoshida S, Stein LR, Grozio A, Kubota S, Sasaki Y, Redpath P, Migaud ME, Apte RS, Uchida K, Yoshino J, Imai SI. Long-Term Administration of Nicotinamide Mononucleotide Mitigates Age-Associated Physiological Decline in Mice. Cell Metab, 2016; DOI: 10.1016/j.cmet.2016.09.013.
- Shuang Zhou, Xiaoqiang Tang, Hou-Zao Chen. Sirtuins and Insulin Resistance. Front Endocrinol (Lausanne), 2018; DOI: 10.3389/fendo.2018.00748.
- Irie J, Inagaki E, Fujita M, et al. Effect of oral administration of nicotinamide mononucleotide on clinical parameters and nicotinamide metabolite levels in healthy Japanese men, 2019 Nov 2]. Endocr J. 2019;10.1507/endocrj.EJ19-0313. doi:10.1507/endocrj.EJ19-0313