Here’s the short answer to the question of whether intranasal oxytocin works: It does seem to reduce anxiety in some people, especially those with social anxiety disorder, although there are limitations to this effect. But before we get into the details about intranasal oxytocin’s efficacy and limitations, let’s take a moment to discuss why it’s so important that researchers are finally beginning to seriously examine intranasal oxytocin as an intervention tool.
Intranasal oxytocin basics
Oxytocin is a neuropeptide that has long been known for its role in uterine contraction during labor and milk ejection during nursing. However, recent evidence has suggested that it may also play a role in centrally mediated social behaviors. What is the effect of intranasal oxytocin on social behavior? One study showed that oxytocin increased the accuracy of emotion recognition from vocal cues and facial expressions (Guastella et al., 2008). A second study found that oxytocin increased empathy toward socially stressed individuals (Domes et al., 2007). In an fMRI study, Riem et al. (2008) found that activation in regions associated with empathy was heightened when participants inhaled oxytocin compared to placebo.
Why intranasal administration may be ideal
Intranasal administration of drugs has been gaining popularity in recent years due to its potential for improved drug absorption and delivery to the brain. One notable example is the neuropeptide oxytocin, which is known to play a role in social behaviors.
A new study published in the journal Drug Delivery provides strong evidence that intranasal administration of oxytocin can lead to its delivery to the brain. Researchers found that all participants who received a dose of oxytocin via nasal spray reached detectable levels in their cerebrospinal fluid (CSF) within 15 minutes.
The CSF is the liquid surrounding the brain and spinal cord, containing high concentrations of cerebral spinal fluid as well as nutrients and important substances that bathe and protect these tissues. The results provide an initial step towards establishing an effective drug delivery system with fewer side effects than traditional oral administration routes.
Meta-analyses comparing nasal and intravenous administration show similar effects
Studies that have compared the effects of intranasal administration (IN) with intravenous administration (IV) have found similar results, suggesting that IN delivery of oxytocin to the brain is effective.
One meta-analysis looked at 11 studies with a total of 275 participants and found that IN administration was associated with increased social approach behaviors and decreased anxiety-related behaviors, compared to IV administration.
A more recent meta-analysis of 20 studies comparing IN and IV administration in an attempt to identify potential factors influencing treatment outcome included a wide range of disorders: autism spectrum disorder, borderline personality disorder, generalized anxiety disorder, panic disorder, posttraumatic stress disorder, schizophrenia spectrum disorders, and substance use disorders.
The analysis found no significant differences between the two modes of delivery in terms of efficacy.
Intranasal delivery may produce more reliable behavioral outcomes than intravenous
Recent studies have looked at the potential for intranasal delivery of oxytocin as a way to increase levels of the neuropeptide in the brain.
This method may produce more reliable behavioral outcomes than intravenous delivery, due to the fact that it bypasses the blood-brain barrier.
Oxytocin has been shown to play a role in centrally mediated social behaviors, and intranasal delivery may be a way to increase levels of the neuropeptide in the brain to produce desired behavioral effects. One study showed that increasing oxytocin in healthy subjects improved their response to emotional faces, such as fearful or happy expressions.
Intranasal delivery is less invasive than other methods of administration and is unlikely to cause any adverse side effects.
However, further research is needed before conclusions can be drawn about the efficacy of this drug for different populations or different disorders.
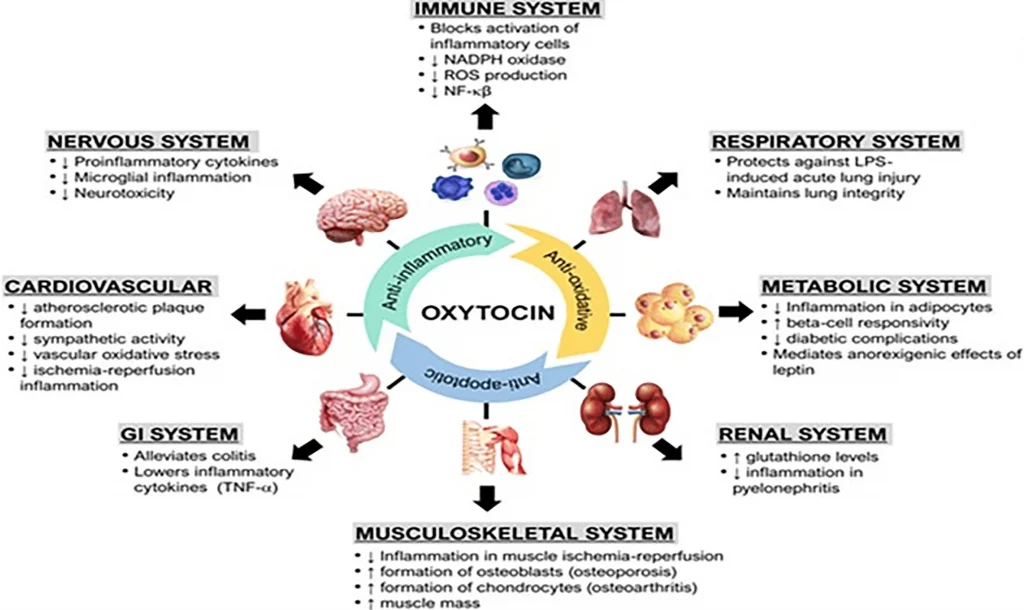
But other factors are important
Intranasal oxytocin delivery to the brain is a hot topic in the research world right now. And for good reason – recent studies have suggested that this method could be an effective way to treat a variety of disorders, from autism to social anxiety. But, as always, there are caveats: While some promising results have been found with intranasal oxytocin delivery to the brain, other factors like dosage and timing may impact whether or not this treatment will work. Researchers are working on better understanding how these factors interact with each other to maximize the effectiveness of this form of therapy.
While intranasal oxytocin delivery has shown promise in delivering therapeutics to the brain, many questions remain unanswered. What role do these drugs play in addiction and substance abuse? How can they best be administered alongside traditional therapies? How can we develop new methods for therapeutic administration?
Potential ways of improving current approaches
The use of intranasal oxytocin has shown promise as a way to improve social behaviors. However, there are a few potential ways to improve current approaches
1) Mixing the drug with another agent such as benzodiazepine or diphenhydramine could reduce the adverse effects of oxytocin
2) Injecting the drug locally
3) Using a nasal catheter instead of an atomizer
4) Developing new formulations for intranasal delivery.
Future research is needed to determine which approach is most effective in various populations. Researchers also need to find out if using intranasal oxytocin can increase its levels in the brain over time. Further research on these questions will help scientists better understand how this drug may be used in clinical practice in years to come.
Future directions based on this review
The administration of intranasal oxytocin has been found to be an effective means of delivery of this neuropeptide to the brain. However, more research is needed to understand the long-term effects of this method of delivery.
Additionally, more research is needed to determine the optimal dose and frequency of administration for desired effects. Given the promising results of this review, future research in this area is warranted. Researchers are encouraged to conduct randomized controlled trials examining the efficacy of intranasal oxytocin as a treatment for social deficits observed in individuals with schizophrenia, autism spectrum disorder, or other developmental disorders.
Furthermore, a continued exploration into how different doses and frequencies of administration may affect both short-term and long-term outcomes will be informative.

